Division of Infectious Diseases
At the end of 2018, we remember and respect Influenza, 100 years after the great pandemic
The Mother of All Pandemics In the 1918-1919 calendar year, the world experienced the worst influenza pandemic in modern times. Coming on the heels of WWI, the H1N1 pandemic occurred in three waves – in the spring of 1918, fall 1918 and spring 1919. Estimates suggest that the pandemic infected a third of the world’s […]
Dec 26, 2018

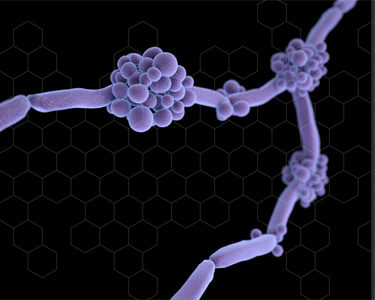
Pharm To Exam Table – Candida glabrata Urinary Tract Infections
The following is a clinical review written by Allison Graner, UNMC College of Pharmacy PharmD candidate 2019, and supervised by Scott Bergman PharmD FIDSA, Clinical Pharmacy Coordinator of Nebraska Medicine Antimicrobial Stewardship Program What is the appropriate treatment for urinary tract infection caused by Candida glabrata? Infections caused by the fungus known as Candida, the […]
Dec 21, 2018
Bacteriocidal versus Bacteriostatic: What Makes the Biggest Difference in VRE Bloodstream Infection?
An October 2018 publication in Critical Care Medicine by Chuang et al details a prospective study of adults in Taiwan, between 2010 -2015, aimed to assess all-cause mortality and rate of bloodstream clearance among patients with vancomycin-resistant enterococci (VRE) treated with daptomycin (bacteriocidal) versus linezolid(bacteriostatic). Patients were treated with conventional daptomycin (6 to < 9 mg/kg […]
Dec 19, 2018
Saving SIRS? Discernment of Sepsis from Non-Infectious Syndromes in the ED
Upon patients’ arrival to the emergency department (ED), determining whether they do or do not have sepsis is difficult. Because of this, many patients receiving antibiotics ultimately are found to have a noninfectious cause of their syndrome. In order to try and improve detection of sepsis in the ED, Mearelli et al. completed a multicenter […]
Dec 10, 2018

Skin Deep: A Closer Look at Treatment of Skin and Soft Tissue Infections
Current guidelines for management of Skin/Soft Tissue Infections (SSTIs) were published in 20141. Nevertheless, management of SSTIs is variable, likely driven by the fact that culture data is often unavailable to direct clinical decision making. Treatment variability results in inappropriate antimicrobial use, highlighting the need for antimicrobial stewardship. Consequently, management of SSTIs is one area […]
Dec 3, 2018

Top 10 Things We Are Thankful for in ID – Letterman Style
Life is better with gratitude. Today, whether or not you celebrate Thanksgiving, we want to continue to show our gratitude and thankfulness to be able to help diagnose, prevent, treat, cure and even advance, the science of medicine. Now, let’s have a little fun! We are grateful for: 10. Hand washing with those cute seasonal […]
Nov 22, 2018

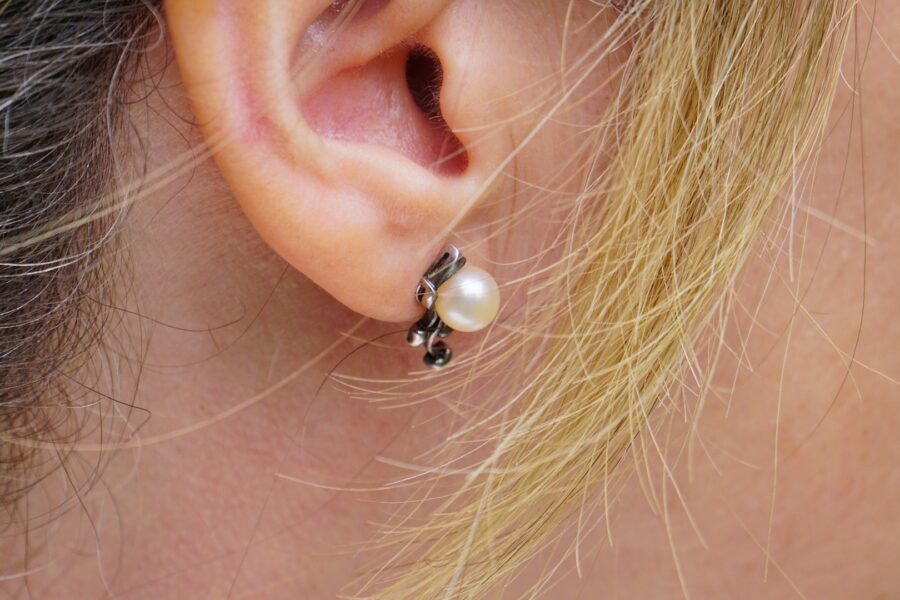
Earrings In Healthcare Workers: Friend or Foe?
Ear piercing among people, including healthcare workers, is a common trend. Katsuse et al, attempted to make a correlation between ear piercings and healthcare-associated infections. In order to prove this relationship, researchers sampled the earlobes and fingers of 200 nurses working at a university hospital. 128 of those nurses had pierced earlobes and 72 of […]
Nov 20, 2018
UNMC Infectious Diseases Fellows are Antibiotics Aware
The following was written by Dr. Raj Karnatak, 2nd year ID fellow at UNMC; a reflection of his current Antimicrobial Stewardship/Infection Control rotation: The UNMC Infectious Diseases fellowship antimicrobial stewardship and infection control rotation provides robust training for fellows in both antimicrobial stewardship and infection control. Training is well designed with education in all the […]
Nov 16, 2018

How Nebraska ASAP is Making Everyone Antibiotic Aware
The following was written by Dr. Salman Ashraf, co-Medical Director of the Nebraska Antimicrobial Stewardship Assessment & Promotion Program (ASAP): Antibiotic Resistance is one of the most urgent threats to the public health. Overuse and misuse of antibiotics allows the development of antibiotic-resistant bacteria. Unfortunately, a significant proportion of antibiotic use in various healthcare settings […]
Nov 15, 2018

Nebraska Medicine is Proud to #BeAntibioticsAware
Our Antimicrobial Stewardship Program (ASP) at Nebraska Medicine has been in place since 2004. Over the years our program has changed and improved sought to expand and improve its approach with the goal of providing extraordinary care to our patients. Rather than an overly restrictive practice, our program has we have emphasized constant regular communication […]
Nov 14, 2018

Recent Posts
- Save the Date: Nebraska Infectious Diseases Conference 2026
- Conference on Retroviruses and Opportunistic Infections (CROI) 2026: Where to find our UNMC ID experts
- New Faculty Spotlight: Dr. Mohanad Al-Obaidi
- Pharmacists in Infectious Diseases: Expertise, Partnership, Impact
- Fast, Accurate, and Practical: Rapid AST for Gram-Negative Bacteremia
Archives
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- August 2025
- July 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- January 2021
- December 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
- December 2018
- November 2018
- October 2018
- September 2018
- August 2018
- July 2018
- June 2018
- May 2018
- April 2018
- March 2018
- February 2018
- January 2018
- December 2017
- November 2017
- October 2017
- September 2017
- August 2017
- July 2017
- June 2017
- May 2017
- April 2017
- March 2017
- February 2017
Categories
- Antibiotic Awareness Week
- Antimicrobial Stewardship
- Bench to Bedside
- Conferences and Presentations
- COVID-19
- Faculty and Staff
- Faculty Recruitment
- Fun With ID
- Guest blog posts
- HIV
- HIV/AIDS
- ICAP
- ID Grand Rounds Speakers
- ID History
- ID Pharmacy
- IDIG
- IDSA
- IDWeek
- In the News
- Infection Prevention and Control
- Journal Club
- Medical Education
- Micro
- Microbe Monday
- NBU
- Nebraska ASAP
- Nebraska ID Society
- Nebraska Medicine ASP
- Oncology ID
- Ortho ID
- Pediatric ID
- PharmToExamTable
- Publication Alert
- Research
- Transplant ID
- Uncategorized
- UNMC ASP
- UNMC Enhanced Medical Education Track
- UNMC ID Achievements
- UNMC ID Fellowship
- UNMC SCC
- UNMCID GIVES BACK
- Weekly Corona
- Why I Love ID
Recent Comments