Division of Infectious Diseases
Get Ready for the Congress of the European Society of Clinical Microbiology and Infectious Diseases (ESCMID)
ESCMID Global, the Congress of the European Society of Clinical Microbiology and Infectious Diseases meeting promises to be a vibrant gathering of thought leaders in global infectious diseases clinical, basic, and translational research. We’re thrilled to highlight the brilliant presenters from our division, each contributing to the advancement of healthcare practices.
Apr 14, 2026

UNMC ID is getting ready for SHEA Spring 2026!
The SHEA Spring 2026 meeting promises to be a vibrant gathering of thought leaders in healthcare epidemiology and infection prevention. Held from April 7-10, 2026, in Chicago, IL, the event will feature groundbreaking research, innovative practices, and insightful discussions. We’re thrilled to highlight the brilliant presenters from our division, each contributing to the advancement of healthcare practices
Apr 3, 2026

Save the Date: Nebraska Infectious Diseases Conference 2026
Mark your calendars—Nebraska’s premier gathering for infectious disease professionals is back on Friday, August 28, 2026, at the Beardmore Event Center in Bellevue. This year brings something new: a fully co-hosted event uniting the Nebraska Infectious Diseases Society and Nebraska ASAP, combining the annual NIDS meeting with the Nebraska Antimicrobial Stewardship Summit.
Mar 10, 2026
Conference on Retroviruses and Opportunistic Infections (CROI) 2026: Where to find our UNMC ID experts
The CROI 2026 meeting promises to be a vibrant gathering of thought leaders in HIV treatment, prevention, and cure research. We’re thrilled to amplify the brilliant presenters from our division, each contributing to the advancement of healthcare practices.
Feb 19, 2026
New Faculty Spotlight: Dr. Mohanad Al-Obaidi
Dr. Mohanad Al-Obaidi joins UNMC ID as an associate professor coming from University of Arizona in Tuscon. His expertise is in care of immunocompromised patients with infections, and fungal infections. Read on to learn more about the newest member of our ID division. Welcome Dr. Al-Obaidi!
Jan 20, 2026
Pharmacists in Infectious Diseases: Expertise, Partnership, Impact
Today, on National Pharmacist Day, we celebrate the incredible contributions of pharmacists to healthcare, and especially to our UNMC ID division. Pharmacists are not only medication experts; they are co-pilots for safe, effective, and equitable ID care. Their impact is especially visible in HIV care and antimicrobial stewardship, where the stakes are high and the […]
Jan 12, 2026

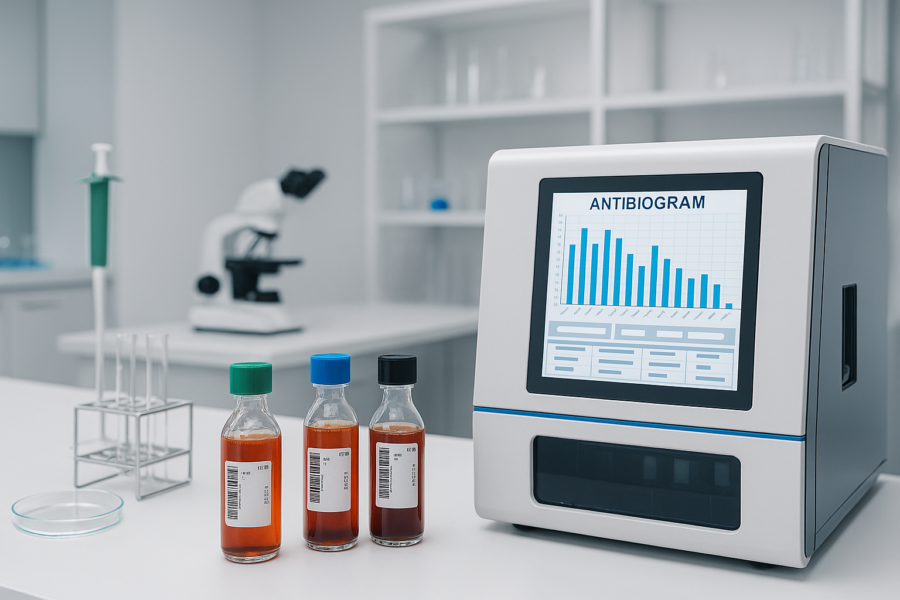
Fast, Accurate, and Practical: Rapid AST for Gram-Negative Bacteremia
Timely and accurate antimicrobial susceptibility testing (AST) is critical for managing bloodstream infections, and delays in initiating appropriate therapy can lead to serious complications. Conventional phenotypic AST, while reliable, can take up to 72 hours to result, and this can mean the difference between recovery and deterioration. Read more about a recent journal club presentation discussing this further!
Jan 8, 2026
2025 Reflections From ID Chief – Dr. Warren
As this year comes to a close, I want to reflect on my (almost) first year serving as Chief of the UNMC Infectious Diseases Division. 2025 started with unexpected changes – Dr. Debra Romberger stepping down from her role as Chair of Internal Medicine and Dr. Mark Rupp taking on the role as Interim Chair. […]
Dec 31, 2025
Year-End Accolades! – We are so PROUD of our people!
Congratulations to members of our division for their achievements and recognitions in the second half of this year! These are just a few of the outstanding accomplishments of our division.
Dec 23, 2025

Understanding Health Misinformation: Why It Spreads, Who It Harms, and What We Can Do About It
By Kelly Cawcutt, MD, MS, FACP, FIDSA, FCCM, FSHEAMedical Director, Acute Care QualitySenior Medical Director, Infection Prevention & Hospital Epidemiology(Adapted from Grand Rounds presentation, December 2025; this post is AI supported creation) Health misinformation isn’t new — but the scale, speed, and impact we’re seeing today is unlike anything in modern history. In 2025, the […]
Dec 16, 2025
Recent Posts
- Get Ready for the Congress of the European Society of Clinical Microbiology and Infectious Diseases (ESCMID)
- UNMC ID is getting ready for SHEA Spring 2026!
- Save the Date: Nebraska Infectious Diseases Conference 2026
- Conference on Retroviruses and Opportunistic Infections (CROI) 2026: Where to find our UNMC ID experts
- New Faculty Spotlight: Dr. Mohanad Al-Obaidi
Archives
- April 2026
- March 2026
- February 2026
- January 2026
- December 2025
- November 2025
- October 2025
- August 2025
- July 2025
- May 2025
- April 2025
- March 2025
- February 2025
- January 2025
- December 2024
- November 2024
- October 2024
- September 2024
- August 2024
- July 2024
- June 2024
- May 2024
- April 2024
- March 2024
- February 2024
- January 2024
- December 2023
- November 2023
- October 2023
- September 2023
- August 2023
- July 2023
- June 2023
- May 2023
- April 2023
- March 2023
- February 2023
- January 2023
- December 2022
- November 2022
- October 2022
- September 2022
- August 2022
- July 2022
- June 2022
- May 2022
- April 2022
- March 2022
- February 2022
- January 2022
- December 2021
- November 2021
- October 2021
- September 2021
- August 2021
- July 2021
- June 2021
- May 2021
- April 2021
- March 2021
- January 2021
- December 2020
- October 2020
- September 2020
- August 2020
- July 2020
- June 2020
- May 2020
- April 2020
- March 2020
- February 2020
- January 2020
- December 2019
- November 2019
- October 2019
- September 2019
- August 2019
- July 2019
- June 2019
- May 2019
- April 2019
- March 2019
- February 2019
- January 2019
- December 2018
- November 2018
- October 2018
- September 2018
- August 2018
- July 2018
- June 2018
- May 2018
- April 2018
- March 2018
- February 2018
- January 2018
- December 2017
- November 2017
- October 2017
- September 2017
- August 2017
- July 2017
- June 2017
- May 2017
- April 2017
- March 2017
- February 2017
Categories
- Antibiotic Awareness Week
- Antimicrobial Stewardship
- Bench to Bedside
- Conferences and Presentations
- COVID-19
- Faculty and Staff
- Faculty Recruitment
- Fun With ID
- Guest blog posts
- HIV
- HIV/AIDS
- ICAP
- ID Grand Rounds Speakers
- ID History
- ID Pharmacy
- IDIG
- IDSA
- IDWeek
- In the News
- Infection Prevention and Control
- Journal Club
- Medical Education
- Micro
- Microbe Monday
- NBU
- Nebraska ASAP
- Nebraska ID Society
- Nebraska Medicine ASP
- Oncology ID
- Ortho ID
- Pediatric ID
- PharmToExamTable
- Publication Alert
- Research
- Transplant ID
- Uncategorized
- UNMC ASP
- UNMC Enhanced Medical Education Track
- UNMC ID Achievements
- UNMC ID Fellowship
- UNMC SCC
- UNMCID GIVES BACK
- Weekly Corona
- Why I Love ID
Recent Comments