Several months ago, a five-person team from Nebraska Medicine’s Biocontainment Unit traveled to Western Uganda, where they trained refugee health workers on appropriate infection prevention and control practices. Dr. James Lawler, one of our Infectious Diseases Faculty, was the team leader on this trip. Dr. Lawler is the Director of International Programs and Innovation for the Global Center for Health Security, and Director of Clinical and Biodefense Research for the National Strategic Research Institute. Dr. Lawler shared his thoughts about the trip with us:
[In Uganda], we were preparing for the seemingly inevitable day when an active case of Ebola virus disease makes its way across the porous border between Uganda and Eastern Democratic Republic of the Congo (DRC) – where the second largest outbreak of Ebola in history continues to smolder along.
Most healthcare workers in top-notch, tertiary-care American hospitals are sufficiently aware and probably don’t need a trip to a developing country to understand how spoiled we are compared to a majority of the world – but most of us don’t realize how constrained we are by working in that environment. As American healthcare becomes more complex and more technologically advanced, its practitioners become more dependent upon advanced systems of care. As our reliance on these systems and technologies increases, our ability to effectively practice becomes more fragile.
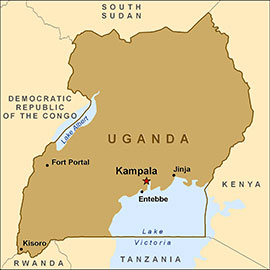
Source: CDC
When thrust into situations where we must teach and perform public health and medicine in resource-constrained settings – where ample supplies of personal protective equipment (PPE), routine laboratory tests, and even running water are often unavailable luxuries – we are forced to return to the basics. The key to effective practice becomes comprehending underlying principles, doing the fundamentals well, and improvising. These skills are important for clinicians and practitioners in all aspects of medicine and public health, and they are invaluable in situations where our sophisticated systems are stretched or fail – such as in rural areas with limited access or in public health emergencies and disasters, where degraded or overwhelmed resources can replicate the austere environment.
The international community should do much more to assist DRC and its neighbors to avert an even greater public health and humanitarian crisis. I am proud of our team and the work that we did. The need for such training is great and the impact potentially important in preventing the continued spread of the ongoing epidemic. Despite this pride, I always walk away from this type of mission with a greater sense of humility and an understanding that we probably learned more than we imparted to our “students.”
Working in the austere environment of rural Africa is well outside our comfort zone as American healthcare workers – and that is the best environment in which to learn. Experience outside of our comfort zone makes us better – better in our daily practice and better in our ability to adapt to the unpredictable. I hope we left Uganda a little more able to manage a potential case of Ebola virus disease, but I know we returned with a better biocontainment unit team. I look forward to future opportunities to expand Nebraska Medicine and UNMC’s international engagement and improve our ability to deliver care back home.
Check out this video to learn more about Dr. Lawler and his team’s trip to Uganda. We are proud to have such talented faculty dedicated to global health and international training!
http://https://www.youtube.com/watch?v=BKk4Afxt9tY&feature=youtu.be
