The following is a clinical review written by Ashleigh Grammar, PharmD, a recent graduate of the UNMC College of Pharmacy, and supervised by Scott Bergman PharmD FIDSA, Clinical Pharmacy Coordinator of Nebraska Medicine Antimicrobial Stewardship Program (@bergmanscott)
What is persistent MRSA bacteremia and how is it treated?
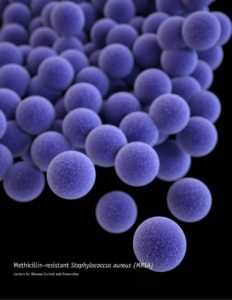 Methicillin-resistant Staphyloccous aureus (MRSA) (photo credit: CDC Public Health Image Library) is a bacteria that can cause a wide variety of infections, including skin or soft tissue infections and bloodstream infections (bacteremia). The Centers for Disease Control (CDC) categorize MRSA as a serious threat (1). Although vancomycin has been a reliable antibiotic to treat MRSA for decades, severe infections from it are still difficult to cure. Current MRSA bacteremia practice guidelines by the Infectious Disease Society of America (IDSA) recommend the use of vancomycin or daptomycin as first-line treatment options for bacteremia (2). Concern arises, however, when bacteremia continues despite the use of these agents. IDSA defines persistent MRSA bacteremia as blood cultures that remain positive after 7 days of effective therapy (2). A study conducted by Cosgrove et al found mortality rates as high as 60% from MRSA bacteremia. Changes in therapy or combination therapy may be necessary despite the limited data (3).
Methicillin-resistant Staphyloccous aureus (MRSA) (photo credit: CDC Public Health Image Library) is a bacteria that can cause a wide variety of infections, including skin or soft tissue infections and bloodstream infections (bacteremia). The Centers for Disease Control (CDC) categorize MRSA as a serious threat (1). Although vancomycin has been a reliable antibiotic to treat MRSA for decades, severe infections from it are still difficult to cure. Current MRSA bacteremia practice guidelines by the Infectious Disease Society of America (IDSA) recommend the use of vancomycin or daptomycin as first-line treatment options for bacteremia (2). Concern arises, however, when bacteremia continues despite the use of these agents. IDSA defines persistent MRSA bacteremia as blood cultures that remain positive after 7 days of effective therapy (2). A study conducted by Cosgrove et al found mortality rates as high as 60% from MRSA bacteremia. Changes in therapy or combination therapy may be necessary despite the limited data (3).
An important step in persistent MRSA bacteremia treatment is identifying all possible sources of infection and obtaining source control through drainage or surgical debridement (3). The IDSA guidelines do not define an optimal treatment regimen for persistent bacteremia. An assessment of the patient’s clinical status around day 7 of therapy is reasonable and should help determine if a change in therapy is warranted. If first-line therapy fails, IDSA guidelines recommend a change in therapy rather than adding an additional agent. Recommendations include high-dose daptomycin at 10 mg/kg daily, if susceptible, in combination with another agent. The second agent could include gentamicin, rifampin, linezolid, sulfamethoxazole-trimethoprim, or a beta-lactam. If there is reduced susceptibility to vancomycin or daptomycin, guidelines suggest sulfamethoxazole-trimethoprim, linezolid, or televancin. These agents could be used alone or in combination with another antibiotic (2). A preferred regimen for persistent bacteremia, however, has yet to be established as most data is only available from case reports or series.
Daptomycin is a cyclic lipopeptide antibiotic that exhibits bactericidal activity against Gram-positive bacteria by inserting its lipophilic tail into the bacterial cell membrane which causes rapid depolarization. In vitro data suggests a synergistic relationship between daptomycin and other antibiotics providing an advantage in persistent MRSA bacteremia. The addition of a beta-lactam to daptomycin improves daptomycin binding to the cell membrane leading to an increase in net cell membrane surface charge and ultimately cell death. A “see-saw effect” also occurs when daptomycin is in combination with an antistaphylococcal beta-lactam where a reduction in daptomycin susceptibility provides an increase in antistaphylococcal susceptibility (3). One case series of 7 patients that were treated with daptomycin 8-10 mg/kg daily plus either nafcillin or oxacillin 2 grams every 4 hours, after failing vancomycin, had blood sterilization within 24-48 hours (4). Adding an antistaphylococcal beta-lactam to daptomycin is a reasonable option when treating persistent MRSA bacteremia.
Similar to the antistaphylococcal penicillins, ceftaroline has also demonstrated a synergistic relationship when added to daptomycin. Ceftaroline, however, provides further benefit by its natural activity against MRSA, vancomycin resistant strains, and daptomycin non-susceptible Staphylococcus aureus. A multi-centered, 26 patient case series reported 96% of patients had clear blood cultures in an average of 2 days after initiation of daptomycin 6-10 mg/kg daily plus ceftaroline 400-600 mg every 8 to 12 hours (5). A recent clinical study of MRSA bacteremia was terminated early due to a significant difference in the mortality rate of daptomycin plus ceftaroline (0%) compared to standard monotherapy (26%), which was mainly vancomycin. Although more data is needed, daptomycin plus ceftaroline has promising results and is an attractive option for salvage therapy in persistent bacteremia.
Another potential option for persistent bacteremia is the addition of sulfamethoxazole-trimethoprim. Combination therapy of daptomycin and sulfamethoxazole-trimethoprim has demonstrated in vitro synergy by increased inhibition of folate synthesis, although the exact mechanism is unknown. The combination did show greater bactericidal activity than either agent alone (7). Two case reports acknowledged successful treatment of a daptomycin non-susceptible bacteremia with daptomycin 10 mg/kg daily plus sulfamethoxazole-trimethoprim 8 mg/kg daily divided every 8 hours (8). In addition, a case series of 26 patients with MRSA bacteremia caused by bone and joint infections identified 24 out of 26 patients that had microbiological eradication in an average of 2.5 days after combination therapy with daptomycin and sulfamethoxazole-trimethoprim (9). This series suggests a potential benefit of this combination in patients that specifically have persistent MRSA bacteremia due to a bone or joint infection.
Although linezolid is an option for S. aureus bacteremia, it is not FDA approved and is often not the preferred agent due to its bacteriostatic activity and large volume of distribution. Combination therapies that add linezolid, however, have shown some benefit in persistent bacteremia. In vitro data has shown a combination of linezolid with daptomycin was more effective than either agent alone.10 Few clinical data have shown this benefit. Two studies demonstrated a 30 day mortality benefit of a linezolid based-regimen over adding another agent to vancomcin (11,12). Although there is a risk of toxicities associated with a prolonged duration of therapy, linezolid based regimens could be used for salvage therapy in persistent bacteremia.
Lastly, rifampin in combination with daptomycin for persistent bacteremia potentially provides additional benefit due to the ability of rifampin to target biofilm. It should be noted that addition of rifampin for bacteremia with endocarditis is not routinely considered because of rapid development of rifampin resistance by circulating S. aureus. Patients with bacteremia due to an infected prosthetic device or bone infections may have more success with this regimen (3). A case series of 12 patients with osteomyelitis or other joint infections showed clinical cure in 10 of the patients that received high dose daptomycin plus rifampin 300-600 mg daily (13). These cases provide another option in salvage therapy for those patients that have an infection with biofilm.
Conclusion
Many combination antibiotic regimens have been shown to be successful in patients that have MRSA bacteremia lasting more than 7 days. Daptomycin-based combinations seem promising. However, the lack of randomized controlled trials and comparative studies has made choosing the most appropriate regimen difficult. The patient’s clinical condition, ability to obtain source control, and results of susceptibility testing should determine when and if a modification to the standard antibiotic therapy is indicated. Because of the significant burden of persistent MRSA bacteremia, antibiotic therapy is warranted for at least 6 weeks. Although a combination regimen is likely not necessary for the full course of therapy, timing of antibiotic de-escalations is also not well studied. Eradication of infection, source control and improvement in the patient’s clinical condition can provide insight as to when de-escalation may be appropriate.

1 comment