by Joe Evans, Nebraska Medicine
A program is being used to help ease physical therapy students into the transition from the academic setting to the clinical environment.
The Early Acute Service Experience program (EASE) helps prepare the students to enter the acute care setting. This program allows students to become more familiar and comfortable managing equipment and communicating with patients before they begin their clinical rotations.
Here’s how the EASE program works:
- Students are assigned a weekend during their second semester to work with a physical therapist at Nebraska Medical Center
- Prior to their assigned weekend, the students complete a module to educate themselves on the experience, what to expect and what is expected of them
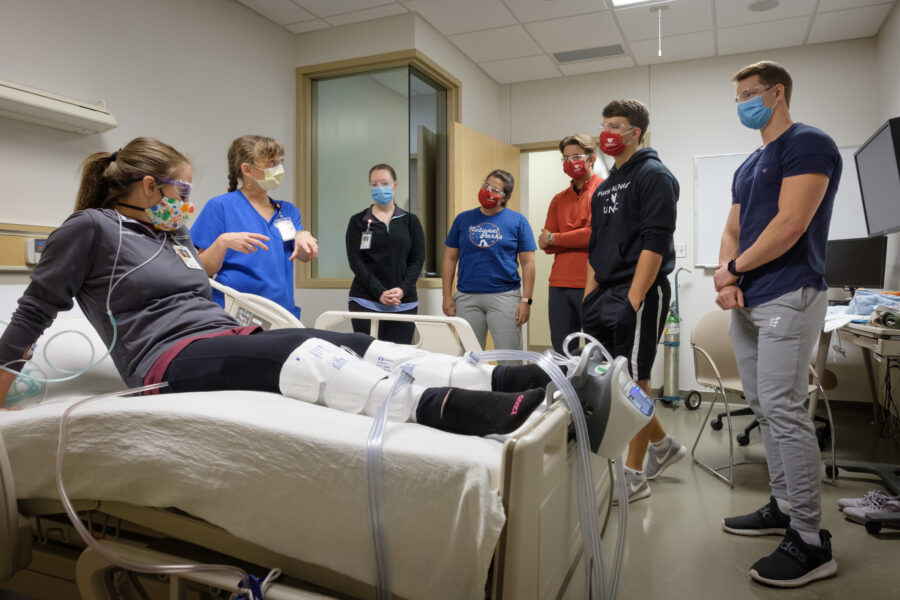
- Students then attend a face-to-face training in the simulation center at the Sorrell Center lead by physical therapist Nikki Sleddens, assistant professor, Director of Clinical Education, and physical therapist Lora Pieper, inpatient rehab supervisor where they are able to practice equipment management (lines, tubes, drains, etc.) and interactions with a simulated patient and therapist including getting out of bed and walking
- The students complete a written reflection following their weekend about their experience
The EASE program came about after conversations between physical therapy teams at UNMC and Nebraska Medicine.
“I had many conversations with the physical therapy faculty at UNMC regarding the challenges students have with the inpatient acute care setting. Many times their clinical rotation at Nebraska Medicine was the first time they stepped foot in a hospital setting,” says Kellie Clapper, manager, Inpatient Rehab Services. “This was not specific to UNMC and Nebraska Medicine, as we saw this with students from the other physical and occupational therapy colleges.”
“Our therapists felt they were spending the first several weeks helping the students develop these skill sets before they could move on and focus on the clinical experience of direct patient care,” says Clapper.
To help with that, the Inpatient Rehab Services student committee developed a “skills box.” The skills box includes items such as chest tube, Foley, oxygen tubing, IV tubing, SCDs, cervical collars, etc. that therapists could use to provide additional instruction to the students outside of direct patient care. A therapist would hook the tubing and braces up to themselves or another therapist to simulate patient care. They would focus on having the students identify the lines and precautions associated with the hospital beds, lines, drains, tubes, and braces and demonstrate how to manage them while getting a patient out of bed and into a chair.
Clapper still wondered, “what if all physical and occupational therapy students had the opportunity to work as an inpatient tech during their schooling?” Her thinking coincided with UNMC Physical Therapy revamping its curriculum. Clapper collaborated with Sleddens and physical therapist Tessa Wells, assistant professor, Assistant Director of Clinical Education, to develop EASE.
Sleddens and Wells say that the UNMC physical therapy program had received feedback from students about how overwhelming it can feel to go from the academic environment to the clinical setting, especially the acute care environment.
“Before the EASE program, students spent the first couple of weeks of the clinical experience orienting to the environment and learning how to manage the equipment versus being able to focus on patient care and clinical decision making,” adds Sleddens.
EASE was launched in January and Sleddens says that feedback from students who have participated in EASE has been very positive.
“When EASE was first presented to the students, they were somewhat reluctant to add a school obligation (outside of studying) to their weekend,” says Sleddens. “However, after their experience, they were grateful for the opportunity and saw the value in, not only gaining exposure to this environment, but also being able to lend a hand to serve clinical partners and start forming professional relationships.”