Public Health in the National News – If you mention “herd immunity” to someone in the agricultural belt of the United States, your conversation will likely turn to livestock. For infectious disease experts, the term means something similar, but it is used in reference to large groups of humans rather than animals. “Herd immunity” and immunization have played a historic role in combating human disease and stabilizing human populations.
History gives us many examples of contagious diseases that decimated populations, for example the plague outbreak in the mid-1300s that came to be known as the “Black Death,” which killed an estimated 30%-60% of Europe’s total population. In the modern era, however, vaccines have helped reduce infectious disease pandemics and stabilize populations. Widespread immunization programs have led to what infectious disease experts refer to as “herd immunity,” meaning that an entire group of people is protected when a large percentage of group members are immune to a particular disease agent. Herd immunity applies to a disease if the following conditions are met:
1) The disease agent is restricted to a single host (i.e., humans)
2) Transmission is relatively direct from person to person
3) Solid immunity against the disease agent is obtained from vaccination or previous infection
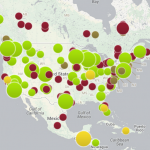
The recent surge in outbreaks of vaccine-preventable disease highlights the complexity and challenges public health agencies face in helping communities achieve herd immunity. Since 2009, there have been over 90 vaccine-preventable outbreaks in the United States alone, accounting for 381 Measles cases, 160 Mumps cases, and over 44,000 cases of whooping cough [1,2]. Roughly 80% of outbreak-associated cases are unimmunized, indicating populations of unvaccinated individuals are a key element of these outbreaks [3].
Barriers to child vaccination include practical issues such as a lack of transportation or money to access vaccinations, and personal concerns such as parents with personal or religious beliefs that oppose vaccinations [4,5]. Emotional or psychological concerns, for example a now-disproven theory that vaccines cause autism, may also cause parents to decide against vaccinating their children. Additionally, a significant number of parents don’t understand the importance of vaccinating their children, are overwhelmed by complex immunization schedules, or find it difficult to make time to complete a full course of vaccinations [6,7].
It is important for care providers and public health practitioners to recognize that people interact with information through their experiences and social settings. Educating parents involves more than providing the facts about the importance of immunization to prevent their children from contracting these infectious diseases and to maintain herd immunity. We must also be ready and willing to address the fears and concerns parents have with vaccinations.
This article was written by John Lowe, PhD, assistant professor in the UNMC COPH Department of Environmental, Occupational, and Agricultural Health, and by KM Monirul Islam, MD, PhD, assistant professor in the UNMC COPH Department of Epidemiology.
[1] Council on Foreign Relations, (2013). Vaccine-Preventable Outbreaks
[2] CDC (2013). Measles – United States, January 1-August 24, 2013. (2013). MMWR Morb Mortal Wkly Rep, 62(36), 741-743. http://www.cdc.gov/mmwr/preview/mmwrhtml/mm6236a5.htm
[3] CDC (2013). Notes from the field: measles outbreak among members of a religious community – Brooklyn, New York, March-June 2013. MMWR Morb Mortal Wkly Rep, 62(36), 752-753.
[4] Dorell, C., Yankey, D., Kennedy, A., & Stokley, S. (2013). Factors That Influence Parental Vaccination Decisions for Adolescents, 13 to 17 Years Old National Immunization Survey–Teen, 2010. Clinical pediatrics, 52(2), 162-170.
[5] Dubé, E., Laberge, C., Guay, M., Bramadat, P., Roy, R., & Bettinger, J. A. (2013). Vaccine hesitancy: An overview. Human vaccines & immunotherapeutics, 9(8), 0-1.
[6] Wick, J. (2011). Removing Barriers to Childhood Immunization. Pharmacy Times. August.
[7] Leask J. (2011). Target the fence-sitters. Nature. 473:443-445.

